2025 Breakthroughs in Polycystic Ovary Syndrome: New Research Reshaping Diagnosis and Care
2025 Breakthroughs in Polycystic Ovary Syndrome: New Research Reshaping Diagnosis and Care
In 2025, polycystic ovary syndrome has emerged as a focal point in women’s health discussions, driven by groundbreaking studies that promise more personalized approaches to a condition affecting millions worldwide. As awareness grows, researchers are uncovering the complexities behind this hormonal disorder, challenging long-held assumptions and highlighting the need for better patient support. This year alone has seen pivotal advancements, from identifying distinct subgroups to genetic discoveries that could lead to targeted therapies, signaling a shift toward precision medicine in reproductive health.
Understanding the Basics of the Condition
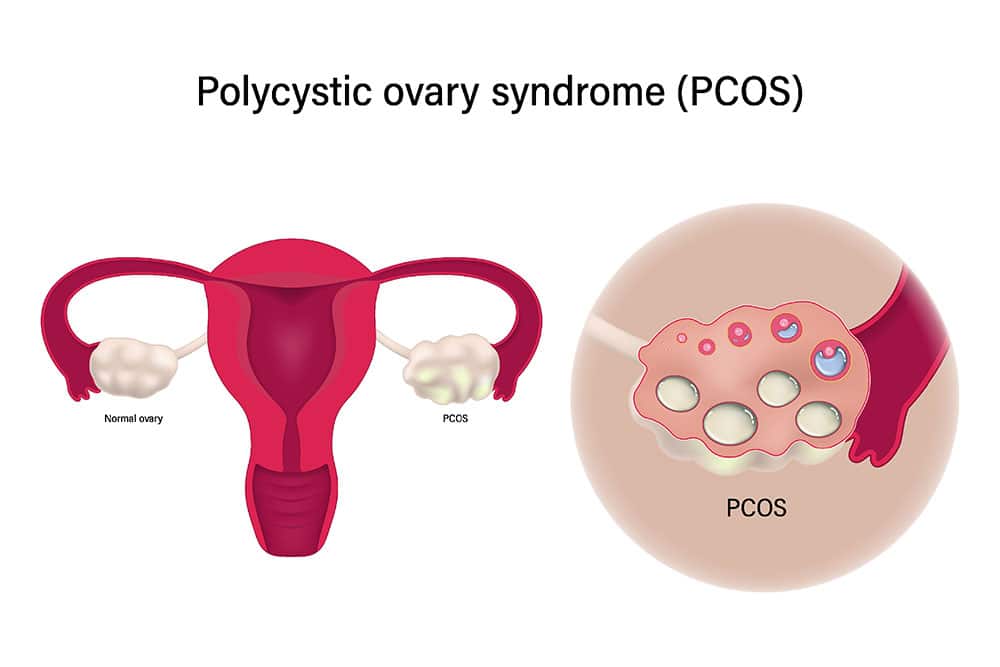
Polycystic ovary syndrome, often abbreviated as PCOS, is a hormonal condition that impacts women during their reproductive years. It typically begins in adolescence, with symptoms that can vary and evolve over time. Common signs include irregular or absent menstrual periods, infertility, acne, excessive hair growth on the face or body, hair thinning, and weight gain, particularly around the abdomen. Beyond these, individuals may experience oily skin or male-pattern baldness.
Those affected are at an increased risk for additional health issues, such as type 2 diabetes, high blood pressure, elevated cholesterol levels, heart disease, and even endometrial cancer. Mental health can also be affected, with higher instances of anxiety, depression, and negative body image. Social stigma related to symptoms like infertility or unwanted hair growth can further complicate daily life, influencing relationships, work, and community engagement.
The exact cause remains unknown, but family history and conditions like type 2 diabetes heighten the risk. It tends to run in families, with variations in presentation across different ethnic groups. Some populations experience higher prevalence and more severe metabolic complications. Diagnosis requires at least two of three criteria: signs of high androgens (like excess hair or elevated testosterone), irregular periods, or polycystic ovaries visible on ultrasound, after ruling out other causes.
Blood tests often reveal elevated levels of testosterone, estrogen, luteinizing hormone, insulin, or anti-müllerian hormone. However, diagnosis can be tricky, as irregular cycles are normal during puberty or menopause, and polycystic ovaries might be hereditary without indicating the syndrome. Worldwide, it affects an estimated 6 to 13 percent of women of reproductive age, making it a leading cause of infertility due to anovulation. Up to 70 percent of cases go undiagnosed, underscoring its status as a significant public health concern.

Patient Voices: Feeling Dismissed in the Healthcare System
A recent study from the University of Colorado Anschutz Medical Campus has shed light on the frustrations many face when seeking help. Published in mid-2025, the research involved focus groups with 24 participants who shared their journeys with diagnosis and treatment. Many reported feeling ignored during adolescence when raising concerns about missed periods, acne, or hair loss, leading to diagnostic delays spanning years.
By the time a diagnosis was made, participants often felt isolated, frustrated, and even blamed for their symptoms. Healthcare providers tended to emphasize weight loss and future fertility, while patients prioritized immediate symptom relief, emotional support, and a deeper understanding of their condition. This mismatch left many to educate themselves through social media and online resources, advocating for tests and bringing information to appointments to gain credibility.
Such self-navigation added stress and exposed individuals to misinformation, prolonging effective care. The study highlights gaps in validation, where symptoms are minimized, and emotional needs overlooked. Recommendations call for a more empathetic, comprehensive approach: listening to patients, providing evidence-based education, and fostering multidisciplinary teams to address the full range of physical and psychological impacts.
The Persistent Misunderstandings Surrounding the Syndrome
Despite its prevalence—affecting one in 10 women of reproductive age globally, including six million in the United States—polycystic ovary syndrome remains one of the most misunderstood women’s health issues. Underfunding is a key factor; classified as an “orphan disorder,” it receives far less research money than comparable conditions. From 2016 to 2022, annual funding averaged $32 million, dwarfed by allocations for rheumatoid arthritis or tuberculosis.
Diagnostic challenges stem from its overlap between reproductive and metabolic domains, not fitting neatly into one specialty. Providers often refer patients to fertility experts, leaving other aspects unaddressed. Many cases are informally diagnosed through conversation without proper testing, and symptoms are downplayed—such as being told irregular periods are normal—leading to feelings of gaslighting.
There is no cure or FDA-approved treatment, relying instead on off-label options like metformin for insulin issues. Inconsistencies in lab standards for hormone tests, like testosterone, result in varying diagnoses. Untreated, it heightens risks for diabetes, hypertension, heart problems, endometrial cancer, and cognitive decline. Multidisciplinary care is ideal but rare, with calls for standardized testing and increased funding to bridge these gaps.
Misinformation thrives online, with unproven supplements like inositol promoted despite lacking robust evidence. Experts warn that such claims outpace guidelines, urging evidence-based management while trials for new options, like low-dose semaglutide, show promise.
Groundbreaking Identification of Distinct Subgroups
In a major development published in Nature Medicine in late October 2025, an international team led by researchers from Karolinska Institutet identified four distinct subgroups within polycystic ovary syndrome. Analyzing clinical data from over 11,900 women across Asia, Europe, and the US, tracked for an average of 6.5 years, the study used standardized measurements to classify patients.
The subgroups are:
- HA-PCOS (Hyperandrogenic phenotype): Characterized by elevated male hormones; linked to higher second-trimester miscarriage risk and abnormal blood lipids.
- OB-PCOS (Overweight-obesity phenotype): Features higher BMI and insulin resistance; associated with the most metabolic problems, lowest live birth rates, but highest recovery potential.
- SHBG-PCOS (High sex hormone-binding globulin): A milder form with fewer fertility issues and the lowest risks for diabetes and hypertension.
- LH-PCOS (Elevated luteinizing and antimüllerian hormones): Highest risk for ovarian hyperstimulation syndrome during IVF; lowest recovery rate.
These categories reveal differences in pregnancy outcomes, complications, and treatment responses. For instance, SHBG-PCOS patients had the best IVF results, while HA-PCOS and OB-PCOS faced more miscarriages and metabolic issues. Tailored strategies, like preferring frozen embryo transfers for HA-PCOS, could improve success rates.
Lead researcher Elisabet Stener-Victorin emphasized the potential for precision medicine: “By identifying subgroups, care can be tailored to each woman’s unique risk profile.” A new web-based tool, PcosX, uses nine measurements to classify patients, paving the way for transformed diagnosis and follow-up.
Genetic Discoveries Paving the Way for New Therapies
Another key study from Mount Sinai and Duke University, published in Nature Communications in August 2025, pinpointed DNA variants in the DENND1A gene that boost testosterone production in affected individuals. PCOS is a complex genetic disorder interacting with environmental factors, making it the top cause of ovulation-related infertility and a major cardiometabolic risk.
Researchers scanned 14 genomic regions linked to the syndrome using high-throughput assays in hormone-producing cells. They identified over 1,000 regulatory elements, focusing on loci like FSHB, GATA4, and DENND1A. Activating DENND1A variants in a cell model increased gene expression and testosterone levels, providing direct evidence of how inherited changes drive hormonal imbalances.
This insight could lead to therapies targeting testosterone at its genetic root, alleviating symptoms like irregular cycles and excess hair. The approach is a proof-of-concept, with plans to expand to more loci and diverse populations to map disrupted pathways fully.
Advances in Treatment and Lifestyle Management
While no cure exists, 2025 has reinforced the value of lifestyle interventions. A review highlighted integrating multiple strategies—like diet, exercise, and stress management—into personalized plans for comprehensive benefits. Weight reduction can lower diabetes risk, and hormonal medications regulate cycles or reduce acne.
For infertility, options include ovulation-stimulating drugs, surgery, or IVF, though risks like hyperstimulation vary by subgroup. Emerging trials explore drugs like semaglutide, but experts caution against unverified remedies amid misinformation.
Guidelines updated this year support using serum anti-müllerian hormone levels over follicle counts for diagnosis, streamlining assessments. Awareness efforts, including September’s PCOS Awareness Month, encourage sharing resources to educate and reduce stigma.
Looking Ahead: A Call for Change
As 2025 draws to a close, these developments underscore the urgency for better funding, standardized care, and patient-centered approaches. By addressing misunderstandings and leveraging new insights, healthcare can evolve to support those living with this chronic condition more effectively.
For reliable information, consult sources like the World Health Organization’s fact sheet on polycystic ovary syndrome. Additionally, explore specialized resources for PCOS to find tailored support and management strategies.
